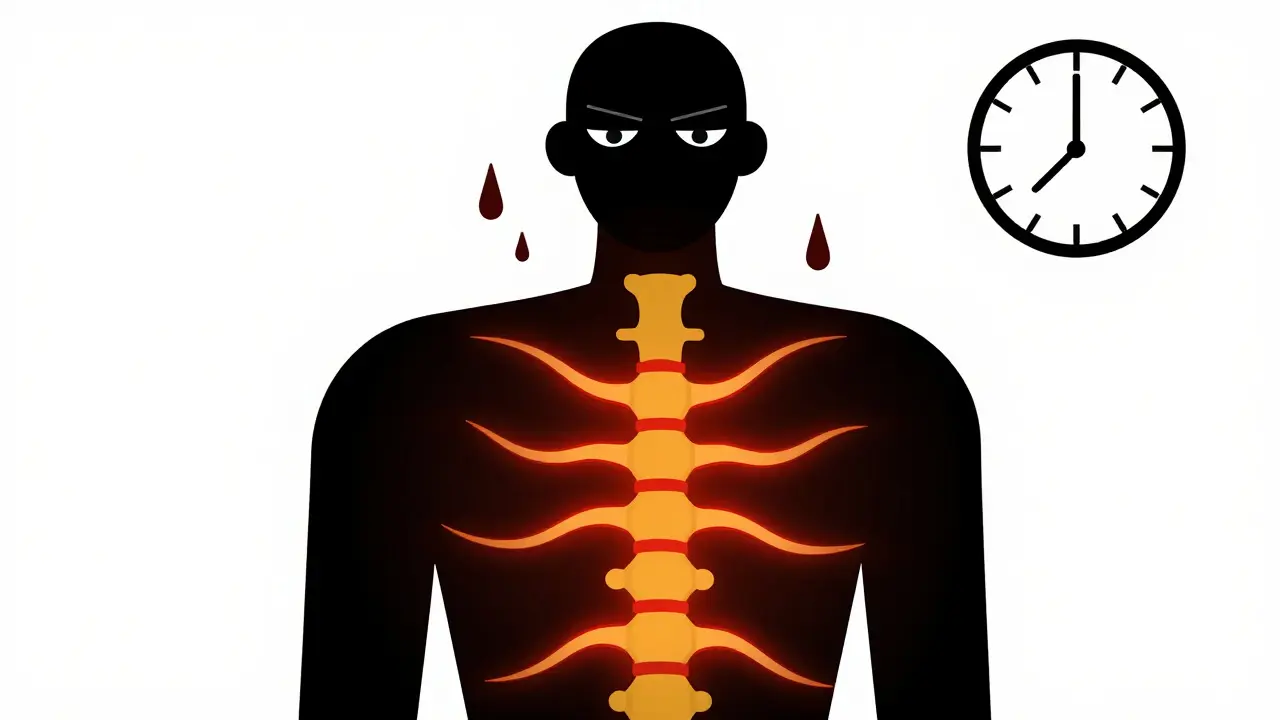
Opioid Withdrawal Timeline Calculator
6–24 hours after last dose
Flu-like symptoms: sweating, nausea, anxiety
48–72 hours after last dose
Severe physical symptoms: muscle pain, tremors, high blood pressure
7–14+ days after last dose
Emotional symptoms: anxiety, cravings, low mood
When someone stops using opioids after relying on them for weeks or months, their body doesn’t just adjust quietly. It fights back. The symptoms hit hard and fast-sweating, chills, nausea, muscle cramps, anxiety, insomnia. It’s not just discomfort. It’s a full-body crisis. And if you or someone you care about is going through this, knowing what to expect and how to handle it can make all the difference.
When Does Opioid Withdrawal Start?
The clock starts ticking as soon as the last dose wears off. But the timing depends entirely on the type of opioid used. Short-acting opioids like heroin, hydrocodone, or immediate-release oxycodone begin triggering withdrawal within 8 to 12 hours. You might notice the first signs: a runny nose, watery eyes, yawning, or restlessness. These are early signals your body is craving the drug.Long-acting opioids like methadone or extended-release oxycodone take longer to leave the system. Withdrawal symptoms here usually don’t appear until 24 to 36 hours after the last dose. That delay can be misleading. People often think they’re fine because they don’t feel sick right away-only to be hit with a wave of intense symptoms later.
The Three Phases of Withdrawal
Opioid withdrawal doesn’t happen all at once. It unfolds in clear stages:- Early Stage (6-24 hours): Flu-like symptoms dominate. You’ll feel achy, sweaty, anxious, and restless. Nausea, vomiting, and diarrhea start. Sleep becomes impossible. This phase is rough, but it’s still manageable with support.
- Peak Stage (48-72 hours): This is the worst. Physical symptoms hit their height: intense muscle pain, trembling, rapid heartbeat, high blood pressure, and extreme cramping. Emotionally, you’re on edge-depression, irritability, and panic attacks are common. Many people relapse here because the discomfort feels unbearable.
- Final Stage (7-14+ days): Physical symptoms begin to fade. But emotional ones linger. Anxiety, low mood, trouble concentrating, and cravings can last for weeks. This is where recovery becomes a mental battle. Without ongoing support, the risk of returning to opioid use spikes.
People using methadone or other long-acting opioids may see symptoms stretch beyond two weeks. That’s normal. It doesn’t mean something’s wrong-it just means the body needed more time to reset.
What Makes Withdrawal So Unbearable?
It’s not just the physical symptoms. Opioids change how your brain processes pleasure and pain. When you stop, your brain is stuck in overdrive. Your nervous system is screaming for balance. That’s why you feel like you’re being torn apart from the inside.Doctors use a tool called the Clinical Opioid Withdrawal Scale (COWS) to measure severity. It checks 11 signs: restlessness, anxiety, pupil size, sweating, tremors, nausea, vomiting, diarrhea, bone or joint pain, goosebumps, and insomnia. Scores range from 0 to 47:
- 5-12: Mild
- 13-24: Moderate
- 25-36: Moderately severe
- 37+: Severe
Knowing your score helps medical teams adjust treatment. A score over 25 usually means you need medication to get through it safely.

How to Manage Symptoms: The Real Solutions
There’s no magic pill, but there are proven strategies that work. And they’re not just about popping pills.Medication-Assisted Treatment (MAT)
The gold standard isn’t toughing it out. It’s using FDA-approved drugs to ease the ride:- Buprenorphine (Suboxone): This is now the most common choice. It reduces withdrawal symptoms by 60-70%. Unlike methadone, it doesn’t cause extreme sedation or respiratory depression. It’s safe, effective, and can be prescribed in a doctor’s office.
- Methadone: Used for decades. It’s strong, long-lasting, and works best in supervised clinics. It doesn’t eliminate withdrawal-it controls it.
- Naltrexone: Blocks opioids entirely. Used after detox, not during. Helps prevent relapse by removing the high if someone uses again.
Here’s something important: You don’t have to go through withdrawal before starting buprenorphine. That old rule-that you need to be sick to get help-is outdated. Experts now say: Start treatment as soon as the person is ready. No suffering required.
Non-Medical Support
Medication helps, but it’s not enough alone.- Hydration: Vomiting and diarrhea drain fluids fast. Drink at least 2.5 liters of water or oral rehydration solution daily. Electrolyte drinks help too.
- Nutrition: Your body needs fuel. Simple meals with protein, complex carbs, and bananas (for potassium) help restore balance.
- Therapy: Cognitive behavioral therapy (CBT) helps manage anxiety and cravings. It’s not just talk-it rewires how your brain responds to stress.
- Acupuncture: A 2019 study found it reduced withdrawal symptoms by 25-30% in most participants. It’s not a cure, but it’s a real tool.
Why Going It Alone Is Dangerous
Some people try to quit cold turkey at home. It’s brave. But it’s also risky.- Dehydration from vomiting and diarrhea can lead to kidney strain or heart rhythm problems.
- Severe electrolyte imbalances happen in 12-15% of unsupervised cases.
- The biggest danger? Relapse. After detox, your tolerance drops fast. If you use the same dose you used before, you’re at 3-5 times higher risk of overdose. That’s not a myth-it’s data.
Medical detox centers don’t just monitor you. They prevent complications. They adjust meds in real time. They keep you safe. That’s why 85-90% of people complete detox with structured care, compared to under 50% without it.
What Happens After Withdrawal?
Detox is just the first step. Withdrawal ends. Recovery doesn’t.Studies show that only 20-25% of people stay off opioids after detox alone. But if they continue with medication-assisted treatment-like buprenorphine or naltrexone-for 6 to 12 months, success rates jump to 40-60%. That’s not a small difference. That’s life-changing.
The goal isn’t just to stop using. It’s to rebuild your life. That means therapy, support groups, stable housing, and purpose. Withdrawal management is the doorway. Long-term care is the path forward.
The Bigger Picture
The opioid treatment market is growing fast. In 2022, it was worth $2.8 billion. By 2027, it’s expected to hit $4.1 billion. Why? Because more people are getting help-and more doctors can now prescribe buprenorphine without special permits thanks to the 2021 MAT Act.But here’s the gap: Only 18% of the 2.7 million Americans with opioid use disorder get evidence-based treatment. That’s not because help doesn’t exist. It’s because access is still uneven. Rural areas, low-income communities, and marginalized groups still struggle to find care.
Changes are happening. The Biden Administration invested $30 million in 2022 to expand services in community health centers. New long-acting buprenorphine formulations are reducing symptoms by 45% in the first 72 hours. Genetic testing might soon predict who responds best to which drug.
But none of that matters if people don’t know they can get help-and that they don’t have to suffer to get it.
Is opioid withdrawal life-threatening?
For healthy adults, opioid withdrawal itself is rarely deadly. But it can lead to dangerous complications like severe dehydration, electrolyte imbalances, or cardiac stress from vomiting and diarrhea. The biggest risk isn’t the withdrawal-it’s what happens after. If someone relapses after detox, their tolerance is gone. A dose they used to take can now be fatal. That’s why medical supervision is critical.
How long does opioid withdrawal last?
It depends on the opioid. For short-acting drugs like heroin or oxycodone, physical symptoms peak at 48-72 hours and fade in 7-10 days. For long-acting opioids like methadone, symptoms can last 14 days or more. Emotional symptoms like anxiety, depression, and cravings often linger for weeks or months. That’s why ongoing treatment is essential-it’s not just about getting through withdrawal, but rebuilding your brain’s response to stress.
Can I detox from opioids at home?
Some people do-but it’s not recommended. Without medical support, you risk dehydration, heart issues, or relapse. Withdrawal symptoms can be overwhelming, and cravings hit hard. Medical detox centers provide hydration, medications to ease symptoms, and monitoring to prevent complications. Even if you feel strong, your body doesn’t know that. Professional care increases your chances of success by nearly double.
Does buprenorphine just replace one addiction with another?
No. Buprenorphine is not a replacement-it’s a treatment. Unlike heroin or oxycodone, it doesn’t cause euphoria at therapeutic doses. It reduces cravings and blocks other opioids from working. People on buprenorphine can work, drive, parent, and live normally. Studies show it cuts relapse rates in half. It’s like insulin for diabetes: it manages a condition, doesn’t cause it.
When should I start medication-assisted treatment?
As soon as you’re ready. You don’t need to go through withdrawal first. That’s an outdated idea. Experts now agree: starting buprenorphine or methadone while still using opioids-even on the same day-is safe and effective. Waiting until you’re sick only delays help. The goal is to reduce harm, not punish suffering.
What’s the best way to avoid relapse after detox?
Continue treatment. Studies show that people who stay on medication-assisted treatment for 6-12 months after detox are twice as likely to stay off opioids. Combine that with counseling, peer support, and stable housing, and your odds improve even more. Relapse isn’t failure-it’s part of recovery for many. But with ongoing support, you don’t have to go through it alone.